The impact of parental responses upon child pain behavior and the moderating role of parental distress
Just imagine, going to a medical practice with your child for an injection. Or for those of you that are not a parent yet, go back in time for a second and think of a moment you remember going for a puncture procedure yourself with your mother or father.
How do you behave as a parent and how do you feel during the procedure?
Give your opinion here: https://linkto.run/p/09ROTB0O
Follow the results here: https://linkto.run/r/09ROTB0O
Or for the others, how did your parents behave during the procedure?
Give your opinion here: https://linkto.run/p/JVVDKBC9
Follow the results here: https://linkto.run/r/JVVDKBC9
Research has shown that certain types of parental responses may negatively impact child pain outcomes whereas other responses may promote child coping behavior. For instance, findings have shown that parental protective or pain-attending responses contribute to increased child pain and distress (1-8). Conversely, parental non-pain-attending behavior, such as distracting the child with humor, may promote child adaptive coping (9,10).

However, evidence for the impact of these type of parental responses is not unequivocal. An affective-motivational account on interpersonal pain dynamics (11) suggests that parental emotions may underlie differential effects of seemingly similar types of responses with deleterious child outcomes being most pronounced when parental caregiving is driven by self-oriented emotions (i.e., parental distress).
In a very recent study we investigated the moderating role of parental distress in understanding the impact of parental responses (i.e., pain-attending and non-pain-attending responses) upon child pain behavior. Participants consisted of 46 children with leukemia (0.6-15y), undergoing a lumbar puncture or bone marrow aspiration, and one of their parents. Parent-child interactions were videotaped immediately after the procedure and parents reported on experienced personal distress.

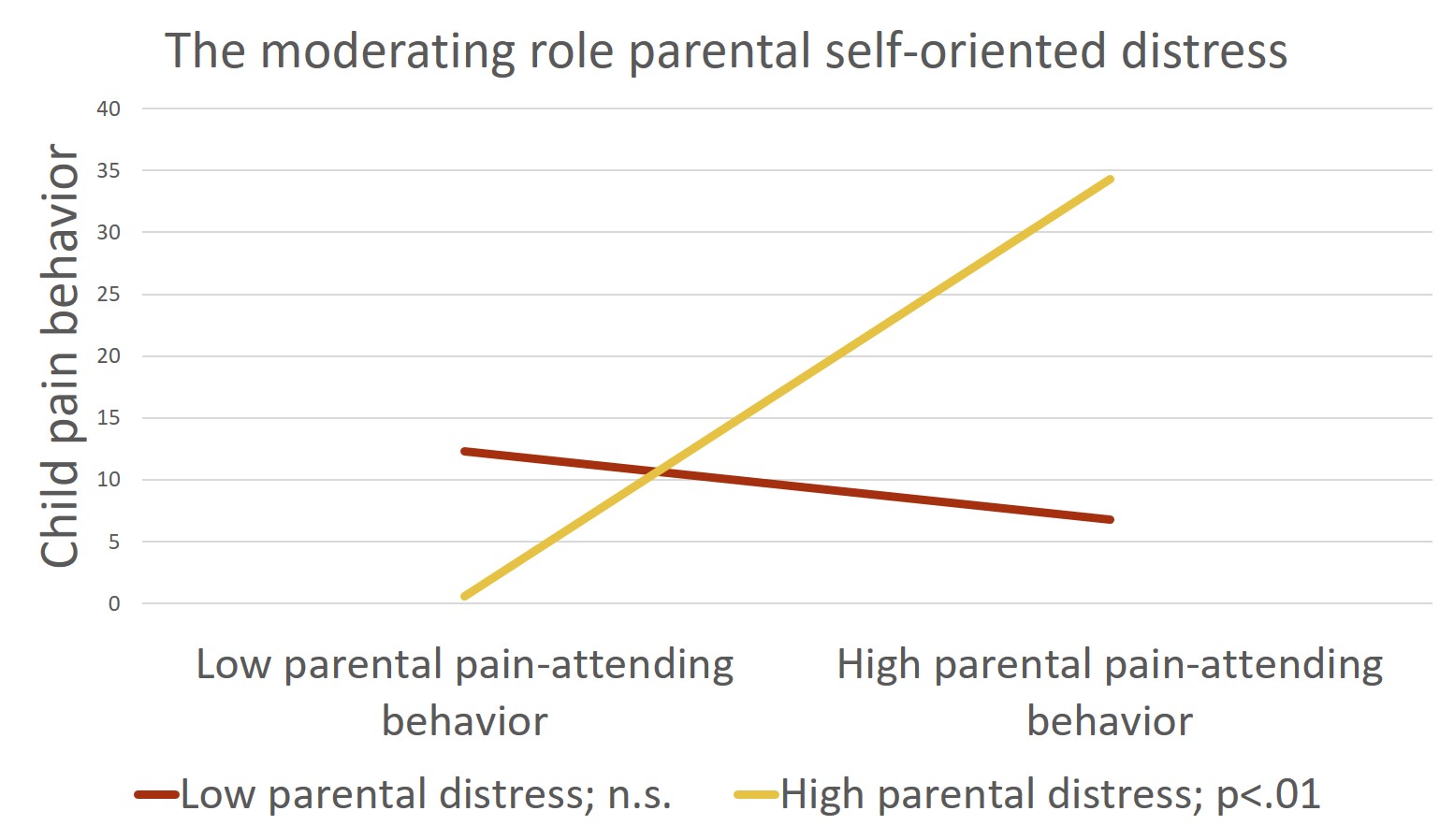
What did we find? Moderation analyses indicated a positive association between parental protective behavior and child pain behavior but only for parents who reported high levels of personal distress. No association was observed amongst parents who reported low levels of distress. Parental non-pain-attending responses contributed to lower child pain behavior, yet this relationship was not moderated by parental self-oriented distress.The current findings point to the critical role of addressing parental emotions as being key to promote more optimal pain-related outcomes.
The current study was recently submitted to Pain Medicine (https://academic.oup.com/painmedicine), so let's all keep our fingers crossed for a smooth publication!
Emma Rheel

Emma works as a doctoral researcher within the Pain in Motion research group and is affiliated to the Department of Physiotherapy, Human Physiology and Anatomy of the Vrije Universiteit Brussel and the Ghent Health Psychology Lab of Ghent University. Her research focus is on the role of distraction, pain neuroscience education and the role of parents in understanding alterations of children's pain and fear memories in children with chronic pain.
2020Pain in Motion
References and further reading:
1. Caes L, Vervoort T, Devos P, Verlooy J, Benoit Y, Goubert L. Parental distress and catastrophic thoughts about child pain: implications for parental protective behavior in the context of child leukemia-related medical procedures. Clin J Pain. 2014;30(9):787-99. https://www.ncbi.nlm.nih.gov/pubmed/24042348
2. Blount RL, Corbin SM, Sturges JW, Wolfe VV, Prater JM, James LD. The relationship between adults' behavior and child coping and distress during BMA/LP procedures: A sequential analysis. Behav Ther. 1989;20(4):585-601. https://psycnet.apa.org/record/1990-10599-001
3. Blount RL, Sturges JW, Powers SW. Analysis of child and adult behavioral variations by phase of medical procedure. Behav Ther. 1990;21(1):33-48. https://psycnet.apa.org/record/1990-18055-001
4. Dahlquist LM, Power TG, Cox CN, Fernbach DJ. Parenting and child distress during cancer procedures: a multidimensional assessment. Child Health Care. 1994;23(3):149-66. https://www.ncbi.nlm.nih.gov/pubmed/10136934
5. Spagrud LJ, von Baeyer CL, Ali K, Mpofu C, Fennell LP, Friesen K, et al. Pain, distress, and adult-child interaction during venipuncture in pediatric oncology: an examination of three types of venous access. J Pain Symptom Manage. 2008;36(2):173-84. https://www.jpsmjournal.com/article/S0885-3924(08)00114-0/pdf
6. McMurtry CM, McGrath PJ, Asp E, Chambers CT. Parental reassurance and pediatric procedural pain: a linguistic description. J Pain. 2007;8(2):95-101. https://www.ncbi.nlm.nih.gov/pubmed/16949882
7. Simons LE, Claar RL, Logan DL. Chronic pain in adolescence: parental responses, adolescent coping, and their impact on adolescent's pain behaviors. J Pediatr Psychol. 2008;33(8):894-904. https://www.ncbi.nlm.nih.gov/pubmed/18375447
8. Blount RL, Devine KA, Cheng PS, Simons LE, Hayutin L. The impact of adult behaviors and vocalizations on infant distress during immunizations. J Pediatr Psychol.2008;33(10):1163-74. https://www.ncbi.nlm.nih.gov/pubmed/18375966
9. Blount RL, Cohen LL, Frank NC, Bachanas PJ, Smith AJ, Manimala MR, et al. The Child-Adult Medical Procedure Interaction Scale-Revised: an assessment of validity. J Pediatr Psychol. 1997;22(1):73-88. https://watermark.silverchair.com/22-1-73.pdf
10. Gonzalez JC, Routh DK, Armstrong FD. Effects of maternal distraction versus reassurance on children's reactions to injections. J Pediatr Psychol. 1993;18(5):593-604. https://www.ncbi.nlm.nih.gov/pubmed/8295082
11. Vervoort T, Trost Z. Examining Affective-Motivational Dynamics and Behavioral Implications Within The Interpersonal Context of Pain. J Pain. 2017;18(10):1174-83. https://www.ncbi.nlm.nih.gov/pubmed/29309272